Post Partum Depression is a complicated mix of physical, mental, and behavioural changes that some women experience after having baby. PPD is a type of serious depression that occurs within four weeks following birth, according to the DSM-5, a guidebook used to identify mental disorders. The intensity of the depression, as well as the amount of time between birth and beginning, are used to diagnose postpartum depression.
Postpartum depression arises after a woman gives birth and is characterized by a persistently poor mood. It is not the same as the “baby blues” that many new parents go through.

Symptoms
At first, postpartum depression may be confused with the baby blues, but the signs and symptoms are more severe and stay longer, and they can interfere with your ability to care for your infant and perform other everyday duties. Symptoms normally appear within the first several weeks after delivery, although they might appear earlier in pregnancy or later — up to a year later.
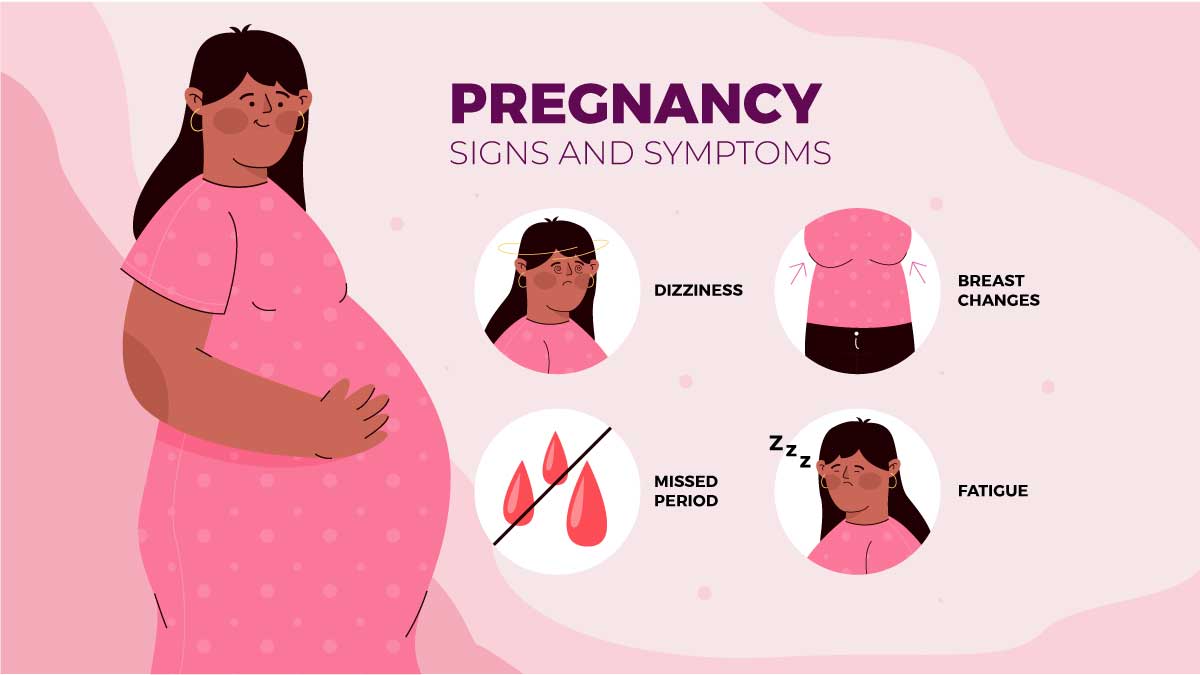
Signs and symptoms of PPD are:
- Depressed mood or mood swings
- Excessive Crying
- Bonding with your infant is difficult.
- Withdrawing with friends and relatives
- loss of Appetite
- Insomnia or excessive sleeping
- a lack of energy
- Reduced interest and enjoyment in earlier enjoyed activities
- Irritability
- Fear for not being a good mother
- Hopelessness
- Feelings of worthlessness, shame, remorse, or worthlessness
- The ability to think properly, concentrate, or make decisions has deteriorated.
- Restlessness
- Anxiety and panic attacks that are severe
- Suspicion of harming yourself or your child
- Suicide or death thoughts
Causes
Doctors are not sure what causes postpartum depression, but it can strike anyone at any time. Environmental factors, as well as genetic factors, could have a role.
The following factors could make you more vulnerable:
- previous adversity
- alterations in hormones
- a previous diagnosis of depression or bipolar illness, or a family history of depression or bipolar condition
- the physical and psychological strains of childbirth and childcare
- additional pressure at work or at home
- sleeping problems
- feeling befuddled
- feeling unappealing
- having the desire to be a perfect parent but not being able to do so
- not having enough spare time
- having issues with nursing
- May having a problem with drugs or alcohol
- having a special-needs child
- after an unintended pregnancy
- being under the age of 20
- having a lack of family and friend support
- Having experienced difficulties during delivery
- a reliable source
- the infant’s need to be admitted to the hospital
- having a child born prematurely
- having a baby who is underweight at birth
Types
There are three terms that are used to describe how women’s moods can alter after having birth:
Baby Blues
Up to 70% of women experience “baby blues.” You can experience abrupt mood fluctuations, such as being extremely joyful and then extremely depressed. You may be impatient, cranky, restless, worried, lonely, and depressed, and you may cry for no apparent reason. The newborn blues can occur anywhere from a few hours to up to 2 weeks after birth. The baby blues usually do not necessitate medical attention. Joining a new moms’ support group or talking to other mothers can often be beneficial.
Post Partum Depression[PPD]
PPD can strike days, weeks, or months after a baby is born. Not only can PPD occur after the delivery of a first child, but it can also occur following the birth of a second or subsequent child. You can experience feelings that are comparable to the baby blues, such as grief, despair, anxiety, and crankiness, but they are much stronger. PPD makes it difficult to do the tasks you need to perform on a daily basis. You should consult a health care practitioner, such as your OB/GYN or primary care physician if your capacity to function is impaired. This physician can assess your symptoms of depression and devise a treatment plan for you. Symptoms of PPD may worsen if you do not receive treatment. While PPD is a serious illness, it is treatable with medicine and treatment.
Post Partum Psychosis
Postpartum psychosis is a dangerous mental disease that can strike new moms after they give birth. This sickness can strike swiftly, usually during the first three months following a baby’s birth. Women can experience auditory hallucinations (hearing things that aren’t actually happening, such as a person talking) and delusions, which can cause them to lose touch with reality (strongly believing things that are clearly irrational). Visual hallucinations (seeing things that aren’t there) are a rare occurrence. Insomnia (inability to sleep), agitation and anger, pacing, restlessness, and unusual feelings and actions are some of the other signs and symptoms. Postpartum psychosis requires immediate treatment and, in virtually all cases, medication. Women are sometimes admitted to hospitals if they are in danger of injuring themselves or others.
Diagnosis
If a person’s depressive symptoms linger for more than two weeks within a year of giving birth, they should seek medical help.
This is also important for anyone having difficulty caring for themselves or their child.
The doctor will inquire about your symptoms as well as your medical history. They could also ask for blood testing to rule out any other possible causes of depression.
Treatment
Depending on the type of symptoms and severity, postpartum depression is treated differently. Anti-anxiety or antidepressant drugs, psychotherapy, and involvement in a support group for emotional support and education are all alternatives for treatment. In severe cases, an IV of brexanolone (Zulresso), a novel medicine, may be recommended. Admission to the hospital is frequently required.
Don’t think that since you’re breastfeeding, you won’t be able to take medicine for sadness, anxiety, or even psychosis. Consult your physician. Many women take medicine while breastfeeding under the guidance of a doctor. This is a decision that you and your doctor must make together.
Complications
Postpartum depression, if left untreated, can disrupt mother-child bonding and lead to family conflict.
Mother: PPD, if left untreated, can endure for months, progressing to a chronic depressive condition. Postpartum depression raises a woman’s chance of future major depressive episodes, even if she is treated.
Fathers: Postpartum depression can have a cascading effect, putting everyone close to a new infant through emotional pressure when a mother is unhappy, the chances of her husband becoming depressed rises as well. And whether or not their partner is depressed, new dads are already at a higher risk for depression.
Kids: Untreated PPD increases the risk of emotional and behavioral disorders in children, including sleeping and feeding difficulties, excessive crying, and language delays.